Top Links
Journal of Case Reports and Studies
ISSN: 2348-9820
Disseminated Cutaneous Mycobacterium chelonae Infection in a 9.5-Year-Old Girl with Diabetes
Copyright: © 2015 Crisinel PA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Related article at Pubmed, Google Scholar
Mycobacterium chelonae is a fast growing mycobacteria that mainly causes localized cutaneous infections. Disseminated cutaneous infections are quite exclusively seen in immunosuppressed individuals. We present a case of disseminated cutaneous infection in a young diabetic patient. This case underscores the need to consider atypical mycobacterial infections in any patient with culture-negative cutaneous infections resistant to conventional antibiotic treatment.
Keywords: Mycobacterium chelonae, Infectious Complications, Pediatric Diabetes, Mycobacteria
List of Abbreviations: M. chelonae: Mycobacterium chelonae; ATS: American thoracic society; IDSA: Infectious Diseases Society of America
Atypical mycobacterial infections can occur at subcutaneous insulin injection sites. These infections are often misdiagnosed. Herein, we report a case of disseminated cutaneous Mycobacterium chelonae (M. chelonae) infection in a pediatric patient with type 1 diabetes mellitus.
A 9.5-year-old girl with type 1 diabetes presented with an inflammatory nodule of her right buttock at the site of a previous insulin injection. She had been followed since her diagnoses 3 years prior and her diabetes had been well-controlled (most recent HbA1c 7.1%, mean HbA1c over the previous 12 months: 7.9%, insulin requirements: 0.76 U/kg/day). When she presented for evaluation of the nodule she was being treated with an intensified basal bolus insulin regime using insuline lispro and insuline glargine. The patient and the parents reported regular changing of insulin needles and local disinfection at injection site. Over the course of one week, the lesion evolved to an abscess requiring incision and drainage. Classical bacterial cultures remained negative.
Despite oral antibiotic therapy (co-amoxicillin, clindamycin), the infection recurred and similar lesions appeared on both thighs bilaterally over the subsequent weeks, some of which discharging spontaneously (Figure 1). Additional bacterial and fungal cultures of the discharging collection remained negative but mycobacterial culture was positive for M. chelonae. Culture was performed in a mycobacterium growth indicator tube (MGIT) (Becton Dickinson Microbiology Systems) in a modified Middlebrook 7H9 broth and incubated in Bactec MGIT 960. When positive, Ziehl-Neelsen staining was performed in order to confirm the presence of acid-fast bacilli. The identification of the mycobacterial isolates was performed by sequencing and analysis of 16S rRNA, hsp 65 and rpoB genes [1]. Laboratory assessment of immunity (immunoglobulins and complement) was normal. ATS/IDSA guidelines recommend to start with a combination therapy for severe infection [1]. However, as the lesions were limited in their extension, we opted for a monotherapy of clarithromycin (10 mg/kg bid) which could be started about 2 months after the first symptoms (Figure 2). The patients tolerated the regimen well and responded favorably over the next 6-months of treatment without recurrence of lesions.
While several case-reports and one series have been described in adult patients with diabetes (Table 1) [2-5], a pediatric case of M. chelonae infection in relation to type 1 diabetes has not been reported. M. chelonae is a rapidly growing saprophyte mycobacteria found in soil, water, and dust [6] and is typically associated with localized cutaneous or soft-tissue infections. Abscesses, cellulitis and subcutaneous nodules are typically described. Disseminated cutaneous infections are almost exclusively observed in immunosuppressed individuals, as are more severe complications such as osteomyelitis, endocarditis, peritonitis, sepsis, meningitis or pneumonitis [1]. Infection primarily occurs by direct inoculation of the skin with contaminated cosmetic [7] or medical [8] equipment. In the present case, we were unable to culture any of the the injection materials as these products were changed early during the course of the infection. Investigations of the injection techniques did not reveal any other source of infection. The possibility of a host susceptibility to mycobacterial infections (such as a mendelian susceptibility to mycobacterial disease [9]) was estimated to be very low according to the absence of a relevant past history and the good response to treatment. Therefore, no further investigation was done. M. chelonae is usually sensitive to clarithromycin and requires a long course of treatment to obtain a sustained cure [10]. Relapse is common and may indicate antibiotic resistance that can occur during prolonged treatment [11]. Fortunately we did not face problems of resistance, despite the choice of a monotherapy.
This case underscores the need to consider atypical mycobacterial infections in any patient with culture-negative injection site infections resistant to conventional antibiotic treatment.
We thank Andrew Dwyer of the Service of Endocrinology, Diabetology and Metabolism of Lausanne University Hospital, for help in the preparation of this manuscript.
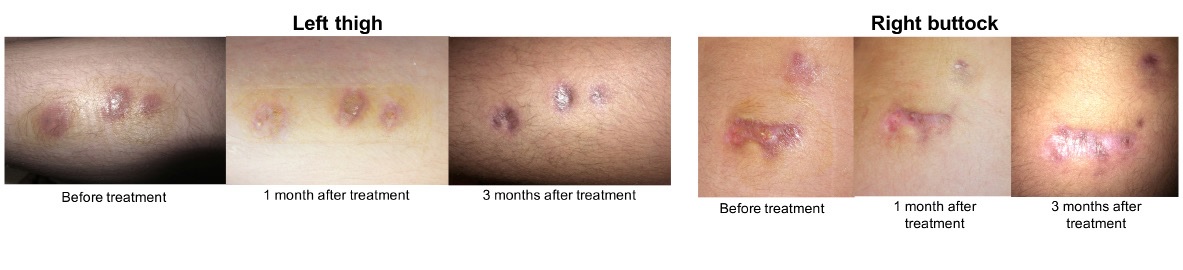 |
| Figure 1: Lesions appeared on both thighs |
 |
| Figure 2: Monotherapy of clarithromycin (10 mg/kg bid) 2 months after the first symptoms |
| Reference | Type of publication | Number of patients | Ages of patients | Type and duration of symptoms before treatment | Antibiotic use and outcome |
| 2 | Case series | 3 diabetic patients out of 100 patients | Unknown | Localized cutanous lesions. Duration unknown | unknown |
| 3 | Case report | 1 | 60 yo | Disseminated cutaneous lesions. 4 months | Doxycyclin, ciprofloxacin, clarithromycin. Complete healing |
| 4 | Case report | 1 | 43 yo | Cutaneous, disseminated. 5 months | Ciprofloxacin, clarithromycin. Complete healing |
| 5 | Case report | 1 | 49 yo | Disseminated cutaneous lesions. 4 months | Clarithromycin, tobramycin. Recurrence of one nodular lesion under treatment before complete healing |
| Footnote: all patients had insulin-dependant diabetes mellitus (either type 1 or 2) and all infections were confined to the skin. Table 1: Case-reports and one series in adult patients with diabetes |
|||||






































