Top Links
Journal of Case Reports and Studies
ISSN: 2348-9820
Optic Nerve Cavernous Haemangioma as a Rare Cause of Retro-Orbital Pain mimicking Intracranial Aneurysm.
Copyright: © 2014 Doukas A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Related article at Pubmed, Google Scholar
Cavernous haemangiomas of the optic nerve, optic chiasm or optic tract are rare. Usually they present with acute onset of symptoms such as acute decline of visual acuity, headaches, nausea or even decline of the level of consciousness which suggests haemorrhage in or even out of the lesion. Otherwise, they have an insidious clinical pattern with subacute or chronic visual disturbance, diplopia and retro- orbital pain.
We present a case of a 42-year-old male patient with pain behind the left bulbus and progressive unilateral visual loss and hemianopsia who was admitted to our clinic with the possible diagnosis of an aneurysm of the left internal carotid artery. The diagnostic work up included thin layer MRI, digital angiography and CT wherein the assumed diagnosis was cavernous haemangioma or tumor of the optic nerve. Total excision of the lesion was achieved via a left frontolateral approach resulting in marked improvement of the visual acuity and the visual field. The histological evaluation confirmed the diagnosis of a cavernous haemangioma.
Keywords: Cavernous haemangioma; Optic nerve; Aneurysm; Frontolateral approach
Eye pain, periorbital and retro-orbital pain are common symptoms, with which many patients present to their ophthalmologist or neurologist. There are numerous causes of such symptoms, which sometimes require immediate or at least prompt therapy. Cerebral cavernous malformations are low-flow vascular lesions, which are typically angiographically occult, have an incident of 0.3/0.7% in the general population and account for 10-20% of all vascular malformations [1]. Most of them occur supratentorially, 15% of them are found infratentorially. 5% of the cavernomas are found in the spinal cord extra- or intradurally [2]. Cavernous haemangiomas of the anterior optic pathway are very rare [3] and either present with acute, subacute or chronic symptoms. They are occult vascular malformations which can also have hereditary or sporadic distribution [4].
We present a rare case of cavernous haemangioma of the optic nerve which mimicked an aneurysm of the internal carotid artery or even a tumor, displacing the optic nerve and optic chiasm and causing retro-orbital pain. After total removal of the lesion via a left frontolateral approach, the visual acuity as well as the visual field deficit rapidly improved. The pain disappeared.
A 42-year-old male patient presented to his general practitioner complaining about progressive decline of his visual acuity on the left side and retro-orbital pain. He was further evaluated from an ophthalmologist who diagnosed left upper and lower quadrant visual field deficit. Under the suspicion of a space occupying lesion pressing the optical nerve or chiasm, an MRI was performed. Herein a thrombosed aneurysm of the internal carotid artery was diagnosed and the patient referred to us for further evaluation and treatment. There were no abnormalities of the ocular movement or other neurological deficits noted.
The first diagnostic modality used was an MRI, since a sellar lesion was initially suspected. The results where however inconclusive and because of the configuration of the lesion in the T2 and T1 sequence with contrast medium an aneurysm of the left internal carotid artery was suspected (Figure 1A-E). Thus, a digital subtraction angiography was performed. Neither aneurysm nor arterio-venous malformations could be seen. A CT scan was additionally performed to rule out calcifications. Hence, two hypothetical differential diagnoses were considered; a cavernous haemangioma or a tumor with intralesional hemorhage of the optic nerve.
A left frontolateral approach was selected. The optic nerve was exposed and after dissecting the falciform ligament the entire lesion was exposed. Hemosiderin desposits were not limited to the lesion, but extended to the frontal gyrus suggesting prior repeated hemorrhage. The lesion had the typical appearance of a cavernoma, showing multilobulated, mulberry-like bulging (Figure 2A). A thin layer of overlying Glia was entered, the accompanying hematoma removed. Using a micronerve hook, the cavernoma could be removed from the optic nerve (Figure 2B). The surrounding Optic nerve displayed multiple shaedes of xanthochromia, supporting our impression of prior bleeding episodes. These areas were left untouched.
The postoperative course was uneventful. The MRI confirmed the total removal of the tumor without complications (Figure 3A-C). The visual acuity of the left eye increased from 0.6 to 0.8 only 2 days after the operation. Moreover, a marked improvement of the visual field deficit could be assessed (Figure 4A-D). The retro-orbital pain disappeared.
There are many causes of periorbital and retro-orbital pain which are mostly treated by ophthalmologists but also by neurologists. That is, because not only eye but also intracranial pathologies affecting the optic nerve, can cause pain in the "quiet" eye. Since the pain is usually combined with headaches and visual deficits, the patients are highly concerned and fear the worst diagnosis such as tumors or even brain hemorrhage [5].
The most common etiology includes ocular processes such as open-angle glaucoma, angle-closure glaucoma, corneal disease, uveitis, scleritis and episcleritism intraocular tumors, ocular ischemia, or suprachoroidal hemorrhage. There are also trauma causes being described such as sclera laceration or rupture. Lastly, retina or choroid processes could also provoke such symptoms.
Another category of processes which lead to periorbital pain are those affecting the optic nerve. These are optic neuritis, neuroretinitis, ischemic optic neuropathy or compressive optic neuropathy [6]. The last group is of neurosurgical interest, since they encompass a variety of tumors affecting the optic pathways such as meningiomas, gliomas, craniopharyngiomas, pituitary adenomas, lymphomas, germinomas, nasopharyngeal cancer with intracranial expansion or metastatic tumors. Other causes include local or systematic infections, vascular or tumor processes of the orbita [7,8].
A cavernous haemangioma has to the best of our knowledge until now not been described with the leading symptoms of retro-orbital pain with visual deficits. Cavernous haemangiomas of the optic nerve are rare. The first relevant article was published in 1978 by Fermaglich [9]. In their review of the literature in 2006, Lehner et al. found 42 cases of vascular malformations involving the anterior optic pathways, of which 30 were cavernous haemangiomas [3]. Hempelmann et al. published in 2007 the first case of complete resection of such a lesion which presented with acute haemorrhage in the perimesencephalic cistern and in the white matter of the right frontal lobe [10]. The lesion because of its cystic components was initially assumed to be a craniopharyngioma with intratumoral haemorrhage. Liu and colleagues found in their review 65 cases of cavernous malformations of the optic pathway and hypothalamus [1]. Krings et al., reported in year 2001 of a patient with an aneurysm of the middle cerebral artery and acute intraparenchymal bleeding. The operation which was performed showed that the etiology of the bleeding was not the asymptomatic aneurysm but a cavernous haemangioma which was diagnosed later via MRI [11].
As in our case, the review of Lehner and colleagues revealed a rapid improvement of visual deficits after excision of the lesion in up to 80% of the patients who were operated [3]. Since remnants of the malformation can lead to re-growth and bleeding, it is advisable to completely remove it whenever possible [1]. Gross total resection is the gold standard of therapy of cavernous malformations. Although decompression without complete resection usually leads to visual improvement, the risk of bleeding is not being reduced [1].
In our case the decline of visual acuity was gradual thus permitting a thorough presurgical work-up. In cases of acute symptomatology or in the extreme chiasmal apoplexy, immediate surgery has to be performed to avoid permanent damage to the visual pathway [3,12].
In such cases the commonly available modality is most likely the CT. In other cases with not such acute onset, MRI is the preferred diagnostic study [13]. Especially gradient echo-sequences (T2 weighted images) are sensitive in revealing small haemorrhages and calcium. MRI is especially sensitive in small lesions, which involve for example the cranial nerves [14]. In our case and since the lesion mimicked an aneurysm of the internal carotid artery an angiography was also performed. However, generally MRI is available and in cases where an aneurysm is not being suspected, the angiography provides no additional information except for rare cases of coexisting venous angioma [15].
We see justification in presenting this case in order to reemphasize the necessity of thorough diagnostic evaluation of patients presenting with orbital, periorbital or retro-orbital pain and visual deficits. Pathologies of the optic nerve should always be included as potential diagnosis. In our case a tumor or aneurysm in the proximity of the optic nerve was initially considered. After advanced diagnostic work up however, we attributed the rare leading symptom of retro-orbital pain to a prechiasmatic intra-optic cavernoma. Microsurgical excision of the lesion and decompression of the optic nerve resulted in immediate resolution of the pain. The visual deficits showed marked improvement from post-op day one continuing to almost total resolution in the next few weeks. These results correspond with the literature and show that the best treatment for these lesions is the operative excision with excellent results (Table 1).
Rapid clarification of visual symptoms and retro-orbital pain with MRI scans and total excision of pathologies which compress but not diffusely infiltrate the optic pathways, should always be considered, since the postoperative results are usually very satisfactory and improve the quality of life drastically.
 |
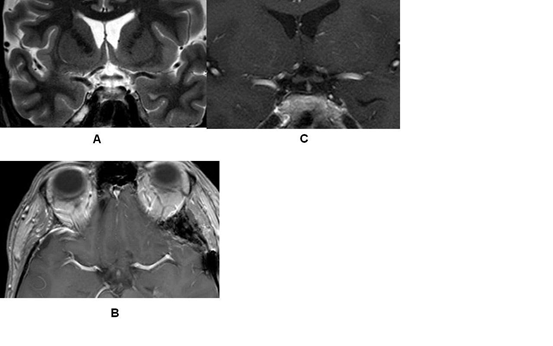
| Figure 1: A. Coronal T2- weighted MRI showing optic nerve being flattened medially and downwards, various fluid intensities B. Axial T1-weighted MRI with contrast medium showing enhancement C. Coronal T1-weighted MRI with contrast medium showing the proximity of the lesion to the internal carotid artery D. Coronal T1-weighted MRI without contrast medium E. Axial CT scan showing hyperdensity of the lesion |
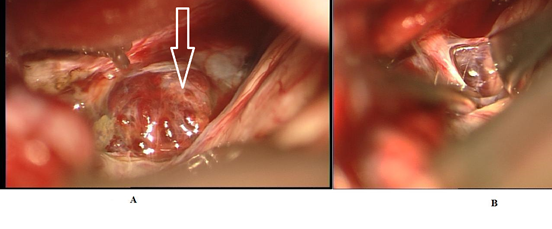 |
| Figure 2: A. Mulberry-like appearance, that extends superiorly from the optic nerve, pushing the optic nerve apart like a wedge (arrow) B. Intraoperative photo after complete resection of the cavernoma. The prior location of the cavernoma is clearly seen, the nerve flattened and broadened by the initial mass |
 |
| Figure 3:
Post-operative MRI confirming the total removal of the lesion A. Coronal T2-weighted MRI with fully recovered normal anatomy of the nerve and chiasm B. Axial T1-weighted MRI post- contrast without residual tumor. On close scrutiny, the previous location of the mass can be still discerned C. Coronal T1-weighted MRI post-contrast |
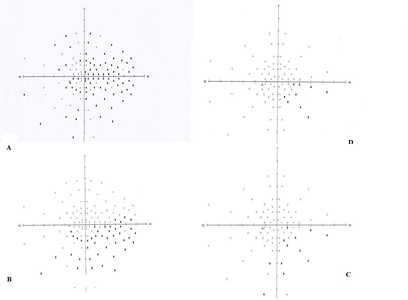 |
| Figure 4: A. Visual field deficit of the left eye preoperatively B. Visual field 2 days after the operation with obvious improvement C. Visual field 3 weeks after the operation 5 weeks after the operation the visual field is almost back to norm D. 5 weeks after the operation the visual field is almost back to normal |
| Authors | Number of cases | Surgical Outcome | Surgical procedure |
|---|---|---|---|
| Liu et al. [1] | 65 | Improvement of visual acuity in 85% | Gross total resection in 60% |
| Lehner et al. [3] | 1 | Improvement | Excision |
| Hempelmann et al. [10] | 1 | Improvement | Excision |
| Lavin et al. [16] | 1 | Improvement | Decompression |
| Mohr et al. [17] | 1 | Improvement | Decompression, biopsy |
| Hassler et al. [15] | 3 | 2 improved, 1 deteriorated | Excision |
| Steinberg et al. [18] | 2 | Improvement | 1 biopsy, 1 laser resection |
| Shibuya et al. [14] | 2 | Improvement | Excision |
| Warner et al. [19] | 1 | Improvement | Excision |
| Iwai et al. [20] | 1 | Improvement | Excision |
| Elmaci et al. [21] | 1 | Improvement | Excision |
| Paladino et al. [22] | 1 | Improvement | Excision |
| Desmukh et al. [23] | 4 | Improvement | Excision |
| Ramina et al. [24] | 1 | Improvement | Excision |
| Son et al. [25] | 1 | Unchanged | Excision |
| Arrue et al. [13] | 3 | Improvement | 1 conservative, 1 excision, 1 partial resection |
| Newmann et al. [12] | 1 | Improvement | Excision |
| Table 1: The table shows other cases of cavernous hemangiomas in the optic pathway, the treatment used and the postoperative outcome of the visual deficit. Notably, there was a marked improvement of the visual acuity in all patients where a total resection was performed. | |||






































